I enjoy blogging. Over a year ago, I commented on how I benefit from blogging, and those comments still hold true.
As part of a recent post, I mentioned taking on new responsibilities at work. I'm trying to do a lot of my old job, train for my new responsibilities, cover for coworkers who are taking big chunks of vacation, and in general deal with the personnel shortages of a company that has laid off half its employees. In other words, I'm spending a lot of time at work.
I'm excited about the direction my job is taking. And I feel lucky I'm able to take advantage of this opportunity: even two months ago, I had neither the physical energy nor the mental capacity for anything so demanding. I am very grateful to have recovered so quickly from my cancer treatments.
The demands of work are requiring sacrifices: I exercise less frequently, I haven't picked back up on my organ lessons, I don't cook what or as often as I would like to, and my blog posts are infrequent. I plan to start picking those things back up after the holidays at the end of 2009. Until then, I will blog only once or twice a month. C'est la vie!
I hope everyone has a happy Thanksgiving!
Saturday, November 7, 2009
Blogging: On hold
Sunday, October 25, 2009
Budgie alarm
My husband and I have two small parrots. Morning with them on most days are pretty quiet: I go to work before the sun comes up, when our birds are still sleeping or engaging in quiet activity.
On weekends, we normally sleep in. For years, when the sun starts shining into our house, our cockatiel would begin a cheeping. A loud "Cheep!," a short pause, another "Cheep!" and on for some time. Often, he would settle when one of us goes into his room. If not, usually having both of us in the living room would get him to calm down.
Why the insistent calls until we get up? I don't know. But it was neat to see that he felt some connection to us.
About a month ago, my husband's coworker found a parakeet at their wild bird feeder. Wilson is now living with us. When a new pet comes into a household, things change.
Parakeets (also called budgerigars, or budgies) are known for talking to themselves. Whistles, cheeps, crackles, words, and any other sounds they learn to imitate get all jumbled up into a monologue. Our first parakeet does this. But Wilson does it much more. Often, when Wilson starts up, the other budgie joins in.
And that's our new weekend wakeup call: the two budgies talking to themselves. No more insistent cockatiel cheeps. I'm a little sad the birds don't seem to need my husband or I as much in the morning. But I'm glad to wake up to such a happy sound: a budgie alarm.
Sunday, October 18, 2009
That's not part of my job!
Growing up, one of my chores was to do the dishes on certain days of the week. A particular day of dishwashing stands out in my mind: after I had done the dishes—completing this chore the same way I had done for years—my father insisted I wasn't finished. "You haven't wiped down the counter!" Passionate argument ensued, with no resolution.
The next day I went to my mother, full of righteous indignation. After hearing my side of the story she said, "Well, it doesn't seem unreasonable for wiping down the counter to be part of doing the dishes."
I don't remember what was said after that: I was overcome by a feeling of dumbfounded shock. No one had ever asked me to wipe down the counter. I was upset at being scolded over a responsibility I had not agreed to; it had never crossed my mind to consider whether the task was reasonable.
At work, I will soon have some authority (although not supervisory) over a number of other employees. Gaining cooperation can be a tricky task; I have heard many supervisors compare their job to parenting. Perhaps memories such as the dishwashing incident will help my management techniques at work.
I hope I'll do well. I'm excited to have the opportunity to try.
Saturday, October 10, 2009
Botanical aid
I complained this spring about an invasive vine threatening my raspberries. I spent a significant amount of time this summer removing the vine from most of my brambles. I was curious about exactly what it was, and took a flowering sample to my local botanical center.
It took several months, but the diligent research of the master gardener paid off: the vine is an American Hog Peanut. Turns out, it's technically a native plant, not an invasive one.
Native plants support significantly more wildlife than imported species. The wildlife in my yard is one of the things I enjoy most about it. So now I don't feel as negatively toward the vine as I did this spring.
I feel lucky to have access to a botanical center with such a helpful master gardener.
Sunday, September 27, 2009
The science of parrots
Sometimes one idea leads to a different idea, one thought to another. The mind wanders.
One of my recent thought trains started with Wilson, a parakeet. One of my partner's coworkers found him at their wild bird feeder. The coworker managed to catch him (the bird let him get within towel-throwing range), and after contacting the local Parrot Society and avian vet (no lost parakeets reported) Wilson now lives with us.
We have two other small parrots, neither of which has ever expressed interest in the noises of radio or television. Wilson, on the other hand, not only gets makes noise in response to the radio, he actually seems to respond to the songs: he gets louder and softer with the music, and often will squawk preferentially on the beats.
The ability to recognize musical beats and perform an action in time with them (such as a squawk or a head bob) is known as entrainment. It used to be believed that only humans had this ability; in April of this year, evidence was published that this is a trait humans share with parrots.
Which in itself is kindof neat. Even more interestingly, the evidence was parrots entraining to the music preferred by their human owners. Other animals can be influenced by musical sounds; a recent study found that the moods of tamarins, a kind of monkey, was affected by music. But not by human music: only by music specially composed to resemble tamarin calls.
It is surprising that parrots, that are such distant relatives (they're not even mammals!), can relate to human music, while much more similar animals (monkeys) cannot. Perhaps the ability to enjoy music of a different species is tied to the ability to make a wide variety of vocalizations. To my knowledge, certain families of birds (parrots and corvids) are the only animals able to imitate human speech.
The ability to make a variety of complex vocalization may correlate to other traits. It was recently suggested that, for evolutionary reasons, complex and varied songs are strongly associated with avian intelligence.
And so it goes, me listening to Wilson cheep while wondering about what evolutionary pressures were shared between his ancestors and mine. I have a wandering mind.
Sunday, September 13, 2009
Red bowl, yellow bowl
Some of our food bowls are red, and some are yellow. When we originally bought the dishes six years ago, it was half and half. When putting away clean dishes, I liked to stack them in alternating piles: red bowl, yellow bowl, red bowl, yellow bowl.
As time has gone one, some bowls have broken. And some get recruited for long-term use (more than a single meal): storing leftovers in the fridge or holding snack foods. I didn't always have an even number of different colored bowls.
The inconsistent color pattern sometimes really bothered me. I have several times rearranged the piles–putting a different color on the bottom–to make the alternating pattern come out. Last week, in exasperation, I changed to single-color stacks. One stack is only red bowls, one stack is only yellow bowls.
I feel good knowing there is now more order in my house.
Radiation summary
For lymphomas, two radiation schedules are common. One is 180 centiGray per day to a total dose of 32 Gray. The other is 150 cGy per day to a total dose of 36 Gy. My radiation oncologist chose to give me the 150/day treatment. He believes the lower daily dose has a lower risk of long-term side effects, even though it requires a higher total dose to be effective. There's not enough good data to make a definitive statement on the issue, but his position sounds reasonable.
My area hospital has a proton radiation machine, so that was what I got. It delivered one dose to my front and one to my back to a about 3.5"-wide strip that started just above my collarbone and extended down my chest about 6". Ideally, they would have treated the entire original area of my bulky tumor. However, the radiation oncologist explained that because radiation to large areas of the lungs is a bad idea, they restricted the width to the mediastinum.
They radiation oncologist and his staff explained to me the most common side effects of radiation to this area: painful swallowing (the esophagus is in the radiation field), coughing (some lung is in the field), and skin damage. I think three different people went over each of these side effects. They gave me a prescription for RadiaGel and told me to apply it three times a day, and to let them know right away if it became painful to swallow because they have drugs that can make that less bad. I think someone might have mentioned being tired was also a possible side effect.
I was more mentally prepared for the physical side effects, I think. They never came: applying the gel twice a day kept my skin from doing anything worse than turning very slightly pink; my esophagus sometimes felt warm and sometimes I felt like it was a very good idea to chew thoroughly before swallowing, but I never had any pain; and I never developed a cough. Two to three weeks into my five-week treatment, however, the fatigue came on.
In part, this was feeling tired and completely unmotivated to do anything productive. I also had to cut back the intensity of my exercise videos: aerobic workouts I had done without trouble two weeks before left me panting with a sky-high heartrate. In addition, I developed an aversion to doing anything that required thinking hard: playing piano, knitting, writing... I had been so happy to enjoy these again after chemotherapy, and they were gone once more.
I'm lucky to have not have any major physical symptoms from the radiation. The surprise of acquiring such intense fatigue made it difficult to appreciate at the time, though. It's easier now (a week and a half out of radiation): I'm not feeling completely normal, but I'm very close. Moving in the right direction.
Tuesday, September 1, 2009
I ate oatmeal today
Some people say to not eat your favorite foods during chemotherapy: it can cause food aversions. Overall, I was lucky to avoid this side effect... except for one food. Since college, oatmeal has been a breakfast staple for me. But somewhere around chemotherapy number seven or eight, I could no longer even bring myself to touch the stuff.
Today, I ate oatmeal. And it was good. It felt like a victory.
Other marks that chemotherapy made are healing: my hair is 1/2" long; what were bright white lines on all eight fingernails are now indistinct lines on just two nails; the frequent pain in my right shoulder has faded to mild discomfort when laying on that side.
Radiation has taken its toll, too. I'm sleeping more than normal and feel tired all day long; even simple tasks like going to the grocery store seem daunting. My exercise tapes have become difficult like they were during chemotherapy. For a while, it also gave me brain fog (difficulty concentrating, "chemo brain").
Even though I'm still receiving radiation (tomorrow is the last of my five weeks of treatments), my brain seems to have recovered some function: over the weekend I tripled the size of the Wikipedia article on hormonal contraceptives. I didn't really believe the radiation oncologist when he said some side effects go away even while one is still receiving radiation; but apparently he was right. While I've been fortunate to avoid physical side effects (such as painful swallowing), some on the lymphoma boards report that those, too, can go away even during treatment.
Next week is exciting for me for two reasons. It will be my first week free of radiation therapy; I'll be completely finished with cancer treatment. And, I'll be restarting work! After two months on layoff, my boss called and said they're ready for me to come back.
The future is looking bright.
Thursday, August 27, 2009
Dead bats and feminism
My project for today was fixing the ductwork for our bathroom ventilation fan. As I posted last week, our original "good enough" installation resulted in a dead bat inside the fan housing.
I thought I was prepared and had everything in the attic I needed to complete the job. But I kept making minimal progress before having to climb out the access hatch and wander around the house looking for tools. I didn't know where any of the tools were, because I think of them as "my husband's tools," and therefore not my responsibility.
During one of these expeditions, a recruiter calls me. Good, I think, another person helping to end my unemployment. "Well," he says, "the job I'm looking at doesn't accept women."
All tools finally collected, I really get down to work in the attic. And discover that self-tapping sheet metal screws require significant assistance to "self-tap." I kept having to take breaks to pant. I wished a man were there to do that part for me.
Near the end of the project, to let me work at a more comfortable angle, I detached the ductwork from the fan. Inside were four dead bats, furry and dessicated-looking. I pondered them for a while. Slowly, it dawned on me that they would have been unable to escape from the vertical portion. It was too small for them to fly out of. It was too large for them to chimney up, and of course too smooth for their claws to get any purchase. Becoming trapped while exploring the ductwork, they must have died of thirst inside it.
With that grim image in my mind, I descended from the attic once more, taking the duct with the bats down with me. I "buried" them in my compost pile, then finished the work that would save future bats from sharing their fate.
Later, I went to my radiation treatment. The techs asked what I had done that day, and I told them I'd fixed the exhaust ducting for my bathroom fan, and found dead bats during my work. "Wow, you must be really handy!" said one woman. The other woman expressed fear of creatures in her attic and commented, "I think my home inspector took pictures of my attic. That's the closest I'll ever get to going inside it!" My doing home repairs and being unafraid of creatures in the attic was not anything they could relate to.
Maybe they would have responded the same way to a man telling that story. But my own feelings of thinking of our tools as "my husband's" and wishing for a "strong man" during the project make me wonder if their reaction was specific to a woman doing these things. After all, as the recruiter reminded me (he was looking to fill a military position), we still live in a world where our gender determines what society expects us to do.
I guess I'll keep working on my own attitude, and trying to be an example of change. One dead bat at a time.
Friday, August 21, 2009
7 Quick Takes (home improvement edition)
The electricians worked all day Monday. And now the contractor's work is all done! We're doing some more work ourselves, but it's exciting to have passed this major milestone.
As electricians work only with wiring and plumbers only with pipes, gutter installers only work with gutters. I'm not sure if this impresses me with the size of the construction industry (that people can make a living working with such a small building part) or with the importance of gutters. Maybe a little of both.
"Of course," he replied. "Just think of the immoral work I would do without you."
Thursday, August 20, 2009
Wikipedia, dashes, and me
Over the past few years, Wikipedians have developed a number of bots and semi-automated processes to fix common errors. I find that I feel like I've been chastised if I make an edit and then a bot immediately comes and cleans up after me; it's become a point of pride with me to try to prevent this.
My efforts to lower the workload of automated computer scripts have given me new habits. One is a compulsion on using hyphens and dashes in certain ways. For example:
I am receiving 36 Gray—at the high end of the recommended range of 32–36 Gy—of proton-beam radiation.Note the hyphen in the compound adjective, the en dash in the number range, and the unspaced em dash in the parenthetical expression. A year ago, I would have just used a hyphen for everything and never thought twice about it. Now I've memorized the HTML codes for the dashes and it would drive me nuts to type something that used them "incorrectly".
Thanks, Wikipedia. I think.
Monday, August 17, 2009
On holiday dates
I have long been somewhat cynical about the date to which Christmas has been assigned. After all, no one knows the time of year in which Jesus was born. A date near the winter solstice was chosen, not based on historical accounts, but to aid in the conversion of pagans who also had major festivals at that time.
I suppose I'd made the assumption that since modern Judaism doesn't actively recruit converts, such considerations were not part of the dates of Jewish holidays. Well, except for Hanuka, which as the "Festival of Lights" has rather obvious midwinter symbolism. But, I rationalized, that's a minor holiday: the book of Maccabees with the Hanuka story isn't even part of the Hebrew Bible.
Learning that the High Holy Days—the Jewish New Year and Yom Kippur—were suspiciously similar to certain Babylonian holidays didn't phase me, either. Celebrating the passing of a year and pondering the ways in which we have gone wrong over the past year are not time-dependent activities. They could be just as meaningful on any date; that the date used by the Jews is the same as that used by the Babylonians doesn't affect the significance of the holidays. Similarly, the way that Easter evolved from Passover has never been something I thought negatively about.
But speaking of Passover, the Bible study I attend is currently studying the Exodus text relating to this holiday. Regarding Passover, the commentaries we use say it used to be two or three separate holidays, none of which was related to freedom from slavery. A date near the spring solstice was chosen, not based on historical accounts, but to institutionalize the telling of the Exodus story by setting it near the date of unrelated pagan festivals.
One of the group members protested, "But Passover has to mean more than that." I come to Bible stories with the belief that they have some basis in truth, but that few details are historically factual. Even so, it bothered me to learn that the date so explicitly spelled out in the text (Exodus 12:18 and 13:4) was chosen for reasons completely unrelated to the story.
I'm not sure if my feelings are rational, or if they are caused by an irrational anti-Christmas, "my husband's holidays are better than your holidays" prejudice. (I specify "my husband's holidays" since I have not converted to Judiasm.) I am very glad, however, to have access to a Bible study group that causes me to think about myself and my assumptions in such interesting ways.
Wednesday, August 12, 2009
History is powerful
I recently finished Battle Cry of Freedom by James McPherson, a history of the civil war. The narrative began with a highly abbreviated description of the Mexican-American war. A striking similarity to our present time immediately drew me into the story: one political party believed that use of troops had spread American freedom and democracy; the other believed American values would have been better spread by being a good example than by military force. The way differences over the Mexican-American war fed into increasing polarization on other issues also felt eerily familiar.
The political situation of the 1850s soon went well beyond our present-day experience, but it continued to tell a powerful story. The experiences of Americans during those years was vividly brought to life. My school history classes had focused on the outcome of the war; reading Battle Cry of Freedom taught me why it was fought in the first place, from the motivations of the leaders to the soldiers to the women and non-soldiers who supported the cause behind the battle lines.
I had been taught that of course the North won, it had a stronger industrial base. McPherson argues that the two sides were evenly matched. Having read through battle after battle where a chance event caused one side or the other to gain advantage, I'm convinced and awed at how easily the war could have gone the other way. I don't think I've ever before read a book that long (900 pages!), but it was a surprisingly easy read, and I'm glad did.
Wednesday, August 5, 2009
Look good, feel better?
I've gone a few weeks now without wearing a scarf. While I'm excited to note that my scalp area has gone from "looks like five o'clock shadow" to "very, very short hair", I'm sure I still present a startling sight to most people.
I appreciate comments along the lines of "you have a nicely-shaped head." Other comments, though also well intended, don't make me feel so good. One person told me, "It's a good thing you look good bald!" As if my right to leave my house without a scarf is dependent on my appearing attractive while scarfless.
In a recent email discussion, I expressed sympathies for a friend with prostate cancer. He was rather retiring about his diagnosis but commented that "observing a roomful of attractive young ladies wearing head scarves and baseball caps" was a "misfortune".
I have been interested recently in the idea that a social system can exist that results in certain outcomes that none of its participants intend. I believe these comments are an example of such a system: the people I quoted above were intending to convey admiration and sympathy. But the language available to them for doing that was limited, and the word choice they made resulted in them reinforcing the social concept that, for women, "value=physical attractiveness".
It's not really what I expected when I went out without a scarf.
Thursday, July 30, 2009
Why the plagues?
My Bible study group recently went through the plague story in Exodus. One theme that kept surfacing was that of attitude toward miracles: the miracles of the plagues are presented as dramatic evidence of God's will. And yet in modern Judaism, as explained by the midrash The Snake Oven, miracles are rejected as evidence of God's will.
In Deuteronomy 30, where Moses is explaining the importance of following God's laws, verse 12 states that a record of these laws "is not found in heaven." The Jewish understanding is that God gave Torah on Mount Sinai, and the post-Sinai interpretation has been entrusted to Jewish scholars: God has agreed to stay out of it.
The Exodus story is so important in Judaism that it has a major holiday devoted to it: Passover. Our study group found the prominence of the plagues in this story to be a stark contrast to the religion's current anti-miracle stance.
The first time this question came up, our rabbi pointed out that the Passover holiday emphasizes the "journey to freedom" aspect of the story, and the plagues get only a minor mention. This consideration lessens the seeming contradiction, but doesn't eliminate it entirely.
Later, we discussed a more interesting possible explanation: in Exodus 10:2, God explains that he causes the plagues so that (as translated by the Jewish Publication Society) the Jewish people will recount the story "in the hearing of your sons and of your sons' sons... in order that you may know that I am the Lord."
At Passover, the Exodus story is recounted in the presence of children. This practice is widespread even among otherwise non-observant Jews: Passover is the most widely celebrated Jewish holiday. The dramatic story of the plagues has motivated generation after generation of parents to tell their children about God's power. If that was their purpose, then the plagues have been wildly successful.
Tuesday, July 28, 2009
Hickman out!
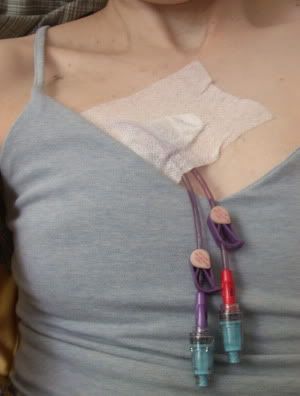 At the beginning of January, I had a Hickman line installed. I wrote some about it here. The line exited my skin in the mid-right area of my chest; it ran under my skin up to my collarbone; at my collarbone, it entered my subclavical vein. In the photo at right, the scar where it was pushed into my vein is visible near the strap of my tank top.
At the beginning of January, I had a Hickman line installed. I wrote some about it here. The line exited my skin in the mid-right area of my chest; it ran under my skin up to my collarbone; at my collarbone, it entered my subclavical vein. In the photo at right, the scar where it was pushed into my vein is visible near the strap of my tank top.
This line made my chemotherapy treatment safer and saved me from countless needle sticks. I had it for five and a half months. Today, I had it taken out.
While the line placement was done in a hospital operating room with sedation, the removal was done quickly in the surgeon's office. The procedure started with the surgeon injecting the area with lidocaine. There was a cotton sleeve around the line near where it exited my skin; the surgeon opened up the exit point a little so he could see the sleeve. The cotton caused my body to form scar tissue, which is what has held the line in. (The surgeon said they used to hold these lines in with stitches, but have found the cotton-scar tissue method is much more reliable.) He cut the scar tissue away from the line, and then it just pulled right out.
The surgeon put a couple of loose stitches at the exit point. He said he did not stitch it up nicely because the wound was potentially dirty, not something he wanted to seal up. So I'll have a scar there, much like the scar near my collarbone.
When I had the line placed, I lost a lot of movement in my right arm: it was a month before I regained my full range of motion. The surgeon said I would be sore tomorrow when the lidocaine wore off, but that it would be minor and only last for a few days.
Hickman lines are somewhat uncommon; port-a-caths are the most common type of central access line for cancer patients. When people have their ports removed, they often say they got deported. Unfortunately, there are no such cute sayings regarding Hickman lines. Not to dwell on that, though: I'm so happy to not feel like a cyborg anymore!
Discovering light
About a year ago, the light in one of our house's closets stopped working. There seemed to be a problem with the socket. We never got around to fixing it, seemingly content with fumbling around in the dark when we needed something out of it.
At the end of last week, electricians came to our house to activate the wiring in our new living room. In what seems unlikely to be coincidence, this closet light now works again.
Upon discovering this, my partner and I gazed into the lit closet. "Hey, we have an iron!" I said. He says, "Are those my tennis shoes? I didn't know I had tennis shoes!"
It's like Christmas in July.
Wednesday, July 22, 2009
My cancer story
I was diagnosed with primary mediastinal diffuse large B-cell lymphoma in December 2008. After months of vague symptoms, I developed a horrible dry cough. As part of investigating my cough, my doctor ordered a chest CT scan. The images showed a tumor under my breastbone that was over five inches wide.
After six months of chemotherapy, the last part of my cancer treatment was a decision to add radiation to my treatment plan. I wrote two posts about my radiation experience, one during treatment, and one after I was finished.
I hope my story is helpful to others. If you have any comments or questions, feel free to email me; my address is 
Throughout my battle with cancer, I have found a lot of support on the message board community at http://forums.lymphoma.com/. They have a "share your story" thread where I have posted a much more detailed description of my initial symptoms and how I was diagnosed.
Before I knew I had cancer, I wrote several posts where I talked about being tired all the time:
- Feeling better
- A mean sick
- Procrastinating past first frost
- A long fall
- Wheat awareness
- Pericarditis that goes on and on
- New symptoms
During treatment, I had several CT scans and one PET scan to track my progress:I also had some thoughts on residual scar tissue.
A couple of posts (although the subject is so important is should really have more than that) on how much the support of others has meant to me:
Posts about the technology used in my treatment:
- Amazing IV Technology
- Hickman line
- Putting the "DA" in chemo
- Neupogen
- Lifetime limits and EPOCH
- Hickman out!
The bulk of my posts on this topic has been discussions of my side effects:
- EPOCH + R, first round
- "Break" week one
- Alopecia
- A mixed break (week 2)
- Difficulty concentrating
- EPOCH + R, round two
- Break, round two
- Beginning EPOCH+R round 3
- EPOCH + R, round three
- Neuropathy
- EPOCH+R, round four
- EPOCH+R break four: side effect round up
- EPOCH+R, round five
- EPOCH+R, round six
- Minor insomnia
- 7 quick takes
- EPOCH+R, round seven
- EPOCH + R, round eight
- EPOCH+R, recovering from round eight
- Residual effects
I have been extremely lucky to have my insurance cover every cost associated with my care, after just one small snag. There are several active members of the lymphoma message boards who do not have insurance, and their situations are just heartbreaking. I hope that soon everyone will be entitled to the same level of care that I have received.
Residual effects
It will soon be two months since my last dose of chemotherapy. I've had eyebrows for a week now. The hair on my scalp has progressed beyond peach fuzz to actually give a small amount of color (à la "five o'clock shadow"). It's enough I'm trying to get comfortable going out in public without a head covering. I'm not there yet - it still feels like I'm not completely dressed - but practice makes perfect.
My only chemo side effects left seem completely benign: big dark blotches in the center of my big toenails, and white lines on my fingernails. I think the fingernail issue is Muehrcke's lines. At least, I hope so, since I added a picture of my nails to that Wikipedia article.
I also have intermittent pain in my right shoulder and upper chest. This was my first symptom of the tumor, and it never completely resolved. My oncologist said it was probably caused by scar tissue. The latest flare-up has so far lasted almost two weeks, with several days being bad enough I need acetaminophen or ibuprofen to function.
Most days, though, I feel completely normal. Even the hot flashes are close to resolving: the intensity is significantly less, and I'm just have a couple every few days. Hopefully this feeling of normalcy will last a long time.
Tuesday, July 21, 2009
Radiation
I'm all done with chemotherapy, to which I responded well. The next question is, should I have radiation? This is a controversial question for the type of cancer I had (primary mediastinal diffuse large B-cell lymphoma). My oncologist recommended getting a second opinion; he sent me to a lymphoma specialist he works with, Dr. Brian Link in Iowa City.
Dr. Link explained that radiation reduces the risk for relapse by 5-10%, a figure that agreed with my own research. The question is, are the risks of radiation worth that benefit? My tumor was under my breastbone. The major risks of radiation in this location are heart disease and, for women, especially young women, breast cancer.
I have no family history of heart disease or of breast cancer; I also have no risk factors for either disease. Dr. Link explains that he worries most about radiation-induced breast cancer in women in their young twenties and in teenagers. Since I am in my late twenties, he's more comfortable with my level of risk. Because my baseline risk for heart disease and breast cancer are relatively low, he believes the benefits of radiation outweigh the increased risks for those conditions.
Dr. Link also told me that he had colleagues - lymphoma specialists at other institutions - that did not believe radiation should be given in cases like mine. The research data is just not there to support a firm opinion in either direction.
With no good data to guide me, though, it seems prudent to follow the advice of my doctors. Today, I met with my radiation oncologist. He was pretty thorough about explaining all the short-term side effects of radiation treatment.
He said many women getting radiation to the chest worry about breast cancer, but this seemed to only be an issue for teenage women. I mentioned the studies I'd seen of women treated 30-40 years ago that experienced significantly higher rates of breast cancer. I'm aware that treatment in the past 8-12 years has used lower doses of radiation applied to smaller areas of the body. But the long-term affects of radiation don't appear for 15-20 years, so there's no data on how effective the newer treatments are at reducing such risks. "Yes," he replied, "there's no data showing current treatments increase the risk for breast cancer."
The radiation oncologist didn't even mention the risk of heart disease. I guess it's a psychological defense mechanism: he doesn't want to believe he's harming his patients. Oh, well. I need him to be good at giving me radiation, not at deciding whether to use it in the first place.
I will have my setup visit Thursday, and then I'll have treatments every day (Monday through Friday) for five weeks. I've enjoyed the past several weeks of no treatment, and it's disappointing to once again have frequent visits to the hospital. Still, I think these weeks will go by quickly.
Thursday, July 9, 2009
How complicated is paint?
Recently, I was talking to my elderly neighbor about painting. He talked about how he used to be a die-hard paintbrush supporter, but eventually got converted to rollers; we discussed how much of an improvement a good paint job can be to a room; the satisfaction that can come from completing a home project such as painting a room.
He also mentioned that when he and his wife (now deceased) painted a room, she put masking tape to protect areas that shouldn't be painted; he applied the paint. He sounded proud about how they had worked as a team, which I thought was nice.
He went on with a story about how she had painted once; she didn't know to thin the paint before applying it, and the whole wall had to be redone. When that happened, he said, he told her to stick to the taping. For the rest of their marriage, she only taped.
These additional details changed my feeling about the arrangement. Confining herself to taping wasn't her choice - she had wanted to paint. She tried one time, messed up, and understandably her confidence in her abilities was undermined. Instead of supporting her by teaching her which paints had to be thinned and how to thin them, he reinforced her belief that she wasn't capable of the task.
I was sad and angry to realize this. I couldn't think of anything appropriate to say to him, though, so I came and wrote about it here.
Monday, July 6, 2009
A busy day
So far today, I have:
- Completed a workout tape
- Filled the bed of my truck with pruned elm trees
- Cooked a pizza from scratch
- Taken my glassware to the recycling facility
- Gone to the library
- Made 20 edits to Wikipedia articles
- Updated my blog (this is my third post today)
- Filed for unemployment insurance
Raspberries, yum
 I harvested about a cup of raspberries yesterday. They have been bearing for a little over a week, but we had neglected to harvest any before yesterday. Everyone in my household enjoyed some of the berries I picked, including the parrots. (The cockatiel still has red stains on his beak.)
I harvested about a cup of raspberries yesterday. They have been bearing for a little over a week, but we had neglected to harvest any before yesterday. Everyone in my household enjoyed some of the berries I picked, including the parrots. (The cockatiel still has red stains on his beak.)
This harvest is a little later than normal (our raspberries are a June-bearing variety that typically bears in, well, June). But we have had mild temperatures, like last year, and the raspberries are actually fruiting a little earlier than during last year's harvest.
Our raspberry patch in the front yard is going gangbusters: almost all of my cup was taken from there. Our patch in the back, however, has been largely overcome by some kind of invasive ivy. Removing the ivy and keeping it in check looks like a large, labor-intensive project. I hope I'm up to it; losing those raspberry bushes would make me very sad.
Almost there
Background: my May 7th CT scan showed a residual mass of 4.3cm x 1.4cm.
I had a combination PET/CT scan June 25th. The CT scan showed a residual mass of 3.2cm x 1.2cm.
I believe the chances of relapse are much lower if the residual mass is less than 25% of the diameter of the original tumor. At diagnosis, my mass was 12-13 cm across (my CT report from Dec. 22 said 12, my PET/CT report from Dec. 30 said 13). 25% of 13cm is 3.25cm, so I'm right at that size.
The best news is the PET report: while I have "minimal residual uptake" of the tracer in the site under my breastbone, nowhere did I have high enough metabolic activity to be suspicious for active cancer. I believe this means I am in remission!
Next step: July 15th appointment with a lymphoma specialist. Topic of discussion: whether I should have consolidative radiation.
Sunday, June 28, 2009
Patchwork of color
 Most of the rooms in our house are currently off-white. We'd like to repaint them all with somewhat brighter colors; it makes sense to start with our new room.
Most of the rooms in our house are currently off-white. We'd like to repaint them all with somewhat brighter colors; it makes sense to start with our new room.
My husband and I discussed paint chips and agreed on a color. The painters came, and now our new room is the color we agreed on. Neither one of us is completely happy with it.
We don't agree which direction to move, though, so we've bought a couple of samples and are doing test patches.
I think one of these colors will do quite nicely.
Thursday, June 25, 2009
EPOCH+R, recovering from round eight
My platelets were low again the week following my last chemotherapy treatment, but I had no bleeding or bruising: not even the minor issues I had after cycle seven. Also in the first week off the chemo, my hemoglobin dropped to 7.9. Below 8.0 is the normal cut-off for needing a blood transfusion. However, my oncologist had noted in my chart to not transfuse me unless I was symptomatic (which I wasn't), so I got away with no treatment.
Someone from my local blood bank left a message on my answering machine two weeks ago. I had called them and left a voicemail in December, canceling my appointment to donate blood and asking them not to call me: I had lymphoma. It was shortly after I was diagnosed; I was pretty upset. When I returned the call from two weeks ago, I got sent to voicemail. I'm not sure if they were calling to see how I was doing, or to ask me to give blood. Just to cover both bases, I told the voicemail that I was finished with chemotherapy and also that my hemoglobin had recently been 7.9.
The hot flashes had subsided somewhat the first two weeks after cycle eight (still multiple times every day and every night, but less often and less intense). This week, though, they came back at full strength. I've had some minor leg pain (a symptom of neuropathy) a few nights (including last night), but no bone pain, no tongue pain, and no hand-foot syndrome this time. I do have a new pain symptom: since about a week ago, both of my big toenails are tender if the end of my toe is pressed. Each nail also has a big red splotch in the middle of the nail bed. I'm not sure what this is called, but when I asked one of my oncology nurses about it, she said it's a common side effect of chemotherapy.
Recently, I've had trouble trying to sleep for more than a few hours at a time; not every night, but many nights I get to sleep rather easily, only to wake up a two or three hours later. Fall asleep again without a problem, but then wake up again an hour or two later. It's hard to tell how much of this is chemotherapy side effect, and how much is due to my crazy work schedule (three weeks of 3am to 11am, then two weeks of 5am to 1pm, and now they've laid off the night shift entirely so I started 6am to 2pm this week).
My hunger and thirst both came back to normal; I even tried eating some jalapeno potato chips last week, which I hadn't done for several months. It was somewhat painful, though; looks like I need to let my mouth heal for longer before trying more of the spicy foods I used to love.
My pants have been looser (although my weight is still the same); I think I've had water retention for several months that I just recently lost. This week, I'm trying reducing my Metamucil fiber cookies to Monday-Wednesday-Friday. So far, my intestines have not complained. My heartrate has consistently been in the 80s recently, which I find reassuring. I did a workout tape today, a tape that a month ago sent my heart rate up to 200: today it only went up to 170, a much more reasonable range for exercise. Interestingly, I was more out of breath today than I was with the higher heart rate: I'm guessing the faster rate, while hard on my heart, was more effective at delivering oxygen?
I feel like I'm recovering. It feels good.
Saturday, June 20, 2009
Cockatiel feng shui
For several weeks, we've been working on the window in our current living room. This required moving the birdcage next to the bookshelves.
Our cockatiel, who loves small spaces, discovered he could crawl behind a row of books. It was quite neat to watch him scoot into and pop up out of that space. The tap-tapping as he pecked against the bookshelf, the sounds of paper we'd given him being chewed up, and the long strings of happy "awk-awk-awk-awk" were really cute.
However, he was overcome with a fierce need to defend this space from all comers. Since he accessed the bookshelf from the top of his cage, this was also an area he defended. If he was in the cage, we could handle him normally; but on top of the cage, watch out. Whenever we walked near (not even necessarily intending to interact with him), he would jump onto us and bite any exposed skin he could find. Hard.
A few days ago, we finished our work on the window and moved his cage away from the bookshelf. Since then, neither of us has even been threatened with a bite. He spends much less time looking angry (somewhat skinny, crest laid flat) - not just with us, but with the parakeet, too - and more time looking contented (fluffy, crest halfway up). We miss the entertainment of his time behind the books; but he's now picked up an old habit of falling asleep on us. It's a good tradeoff.
It's amazing what a little furniture arrangement can do. Then again, perhaps we shouldn't be surprised that parrots are affected by feng shui. After all, some argue that they invented tai chi.
Sunday, June 7, 2009
EPOCH + R, round eight
Three weeks ago (right when I finished round seven), my company laid off our only night shift inspector. To try to get product ready to ship out on our trucks in the morning, I have been starting work at 3am. I have been leaving work at 11am, which is nice, but makes for a weird sleep schedule (nap when I get home, wake up for the afternoon, then have a short sleep before work). This coming week my boss is having me try a 5am to 1pm shift; it would be nice if that ends up working so I can stop having to wake up at two o'clock in the morning.
At the end of the first break week, my blood tests came back low on platelets. I noticed several times that idle scratching of a scab produced, not a lot of blood, but much more than would have normally seen. My eighth Neupogen shot left me with a bruise, something that had not happened before. It worries me to have my blood cells becoming more affected by the chemotherapy. On the bright side, though, my hemoglobin levels have been hanging in there. Below 12 is anemic; below 8 requires a blood transfusion. The past four cycles, I've squeaked by at 8.3 to 8.4.
I was not hungry or thirsty for most of my first break week. My thirst started working again on Thursday, but the hunger came back more gradually. It wasn't until well into my second break week that I felt I was eating normally again. I must have been making myself eat enough, though, because I did not lose any weight. It's reassuring to be at the same weight I was when I started the chemo.
The break from round seven, for the first time during my treatment, I never felt a need for pain relievers. No nighttime leg cramps, no tongue pain: it was wonderful to be pain-free for so much of the time. That said, I did have some occasional minor irritations. One was similar to lower back pain/cramps I have typically had on the last day of Neupogen shots. This cycle, however, I had cramps along my entire spine (usually when I was leaning forward to look at something) that persisted several days after my last shot. I had been attributing this to the "bone pain" side effect of the Neupogen, but now I think it must be something else.
Also, the palms of my hands and soles of my feet were very sensitive for a couple of days during my second break week (e.g. standing on an uneven surface barefoot was painful). I believe this is called hand-foot syndrome. Having it for a long period of time can cause a person to lose their fingerprints, which apparently upsets U.S. Customs officials. This isn't a risk in my case (since I plan on being done with chemotherapy now), but I thought it was interesting.
My eighth week of chemotherapy was very similar to the past few rounds: sleeping about ten hours a day, toward the end of the week everything started tasting really nasty (on Friday I had the nurses give me IV fluids). The hot flashes have continued. And of course, the torso swelling this weekend that makes it painful to be touched (I think is inflammation caused by withdrawal from the steroids). The lack of hunger and thirst has started, and I know I'll have the low energy/steroid crash in a couple of days. But I'll get through it, and this time, I get to stay feeling normal! Yay for chemotherapy being done!
Sunday, May 31, 2009
Rolling out the dough
When I was in middle and high school, I cooked very little. In college, learning to be responsible for feeding myself was a challenge: grocery shopping, menu planning, the whole works.
Even now, ten years later, I still struggle with some things. Today, I tried a new recipe: spinach calzones. For the first time in my adult life, I used a rolling pin. The first one was rather frustrating: the dough kept sticking to the pin, it was square instead of round, and getting it to the right size took more time than I really wanted to spend on it.
Then a childhood memory came back, of helping my mom roll out dough. I couldn't have been older than ten, but the rhythm has stayed in my brain all these years: roll, roll, flip, roll, roll, flip... my dough wasn't exactly a circle, but it was roundish, it didn't stick to the pin, and things generally seemed to go faster.
Thanks, mom.
Saturday, May 30, 2009
Lifetime limits and EPOCH
One of the drugs in my chemotherapy regimen, doxorubicin, has a lifetime maximum dosage. (This is the H drug in the acronym; its trade name is Adriamycin, and the drug is also known as hydroxydaunorubicin.) According to Wikipedia, this maximum dosage is 550 mg/m2. Above that dosage, there is a high risk of permanent heart damage.
I think, after round eight this week, I will have received a cumulative dose of 510 mg/m2. I asked one of my oncology nurses how close I was to my lifetime limit; she wasn't sure, and asked the doctor. Apparently the maximum dosage is much higher when the drug is given by continuous infusion: most treatment regimens involve giving doxorubicin over just a few hours (2-4?), while in my regimen I receive it over 96 hours. He didn't give specific numbers, but said I was "far away" from any dangerous amount of doxorubicin.
I did some internet searches and came up with a couple of studies confirming what my oncologist said: one of adults, and one of children.
Hopefully, when my treatment is finished in another month or two, I won't have to deal with cancer anymore. But it's reassuring to know that, if I needed it, this particular drug is still an option for me.
Monday, May 25, 2009
Guided by the sky
I learned this week that this is the International Year of Astronomy, celebrating the 400th anniversary of Galileo's telescope and of the publication of Johannes Kepler's Astronomia Nova. As part of their observance of the IYA, the editor's column in this week's Science News discusses a claim by Henri Poincaré that astronomy "has given us a soul capable of comprehending nature."
Apparently Poincaré believed that it was success in the science of astronomy that inspired scientific investigation of other topics. "Under heavens always overcast and starless, the Earth itself would have been for us eternally unintelligible," he wrote.
That's an impressive theory. My knowledge of scientific history is insufficient to judge its merits, although the Science News editor is credulous enough to lend some weight to this claim. I would like to think humanity would have muddled into the realm of science even without the help of the night sky. Still, it's intriguing to think about the stars in their courses showing humans that nature obeys strict laws, and that careful observation can discover those laws.
Many religions assume the universe was created for humanity. In discussions of this assumption, it's sometimes asked why, if humans are the point of the universe, so many stars were created. On the face of it, assuming a human-centric Creator, the size of the universe seems incredibly superfluous. But the "stars as a guide to science" theory offers a nice response.
Cool.
Friday, May 22, 2009
Garlic: high hopes
 After a few years of replanting garlic that hadn't grown very well, last fall I bought new stock from a seed catalog. Unfortunately there's no perspective in my picture, but the garlic is mid-thigh on me. I'd forgotten how big garlic gets when you start with big cloves!
After a few years of replanting garlic that hadn't grown very well, last fall I bought new stock from a seed catalog. Unfortunately there's no perspective in my picture, but the garlic is mid-thigh on me. I'd forgotten how big garlic gets when you start with big cloves!
My plan is to use Miracle Grow on it once a week until the summer solstice. (Garlic is day-length sensitive and won't grow any once the solstice is past.) With the remodeling and my chemotherapy treatments, the garlic is the only gardening I'm doing this year. I hope those bulbs get as big as their green tops!
Tuesday, May 19, 2009
Spinach revelation
I try to cook with spinach regularly: being vegetarian, iron deficiency is an issue for me, and my body seems to absorb iron from spinach better than any other food. I have for years (my entire grocery shopping career) bought frozen spinach as a block.
At my last grocery shopping trip, the store was out of the frozen spinach blocks. Nothing, not even way back on the shelf where only my husband can reach. Searching through the frozen vegetables section, I find frozen spinach in a bag. A bag of frozen spinach? It struck me as so odd. But I got two.
I can't believe I haven't discovered this before: I can use just half the bag without the assistance of a bread knife. I can stir the pieces of spinach into my dish without having to wait for the entire mass to melt. The pieces melt faster than a block does, too! Why would anyone buy a frozen block when bagged pieces are available?
There must be some advantage to the blocks. But as for me, I am a convert to the way of the bag.
Remodeling excitement
 Our new vinyl siding is going up. We liked the color of our house, and matched it as closely to our old siding as we could. It does mean no "new house color" excitement. But it's nice to see the insulation being added to our house, and to know we won't have any future need for paint.
Our new vinyl siding is going up. We liked the color of our house, and matched it as closely to our old siding as we could. It does mean no "new house color" excitement. But it's nice to see the insulation being added to our house, and to know we won't have any future need for paint.
Except for the siding, our porch is finished. We've had years of mild fear that our porch would sink into the ground and take part of the house with it. Now, it's obviously still a construction zone, but we have a structurally sound porch!
I haven't taken any pictures, but the drywall is up in our south living room, too. It not only makes it look more like a room than it did at my last update, it stopped all the off-dusting from the cellulose insulation. Ah, clear air! I had written in that update that our roof was finished, complete with removal of our badly-damaged gutters. I got ahead of myself, though: the gutters have not yet been replaced. And our basement is suffering. The damp areas in this photograph? This weekend had a half inch of standing water.
I had written in that update that our roof was finished, complete with removal of our badly-damaged gutters. I got ahead of myself, though: the gutters have not yet been replaced. And our basement is suffering. The damp areas in this photograph? This weekend had a half inch of standing water.
It's not dampening our excitement over the progress, though. What an exciting summer.
Sunday, May 17, 2009
Not alone
I have been touched by so many people in the past months. My family has given me exactly what I needed from them: at different times talking, listening, and giving me space. Caring and supportive messages from so many people I've met only over the internet have buoyed me.
Members of a knitting group I attend put together an amazing care package that has been helping to keep me warm, clean, fed, and entertained. My mother put it best when she said it gave an environment surrounded by love.
Members at my synagogue have called and written and offered support. Friends have helped me focus on fun things that have nothing to do with cancer.
I don't think there's any way to repay everything that has been done for me. This is such a short post for such an important topic, but I hope all those who care for me know this: it means the world to me to not be alone.
EPOCH+R, round seven
Well, first for some backtracking. After cycle five, I had written that my leg cramps had cleared up. I think it was only minutes after posting that I got leg cramps again. Cycle six they came back during the second break week, but instead of diffuse cramp-type pains, my calves just decided they wanted to be shorter. Sitting or standing straight up was fine, but leaning forward to take a step? Ouch. Going downstairs was the worst - I had to keep most of my weight on the handrail for a few days.
The pain from my last round of Neupogen shots was minimal - no need for acetaminophen, even at night. I had none of the pain from breathing or leaning forward, and no esophagus tingling, either. I still had a few days where eating made my upper chest awfully uncomfortable, though. Oddly, some foods went down better than others: Tuesday of my first break week my dinner was no-salt potato chips and ice cream.
In the days after cycle six, the bottom of my tongue ached when I first got up. Thursday of that week it didn't stop. The numbing mouthwash helped a lot with eating: no mouth pain, and it reduced the pain of swallowing (although it wore off after about twenty minutes and sometimes I had to re-dose mid-meal). The tongue pain was not intense when not eating, but it bothered me enough I had to take acetaminophen or ibuprofen to get to sleep - and then I would wake up in the middle of the night and have to take pain meds again. It wasn't until the following Monday that all that cleared up.
My blood counts before cycle seven were still good, but worse than they've been before any other cycle. I guess my bone marrow is getting worn down. Happily, my thirst kept working throughout my break of cycle six and until Thursday of cycle seven. At that point, though, the awful taste in my mouth came back. I had the nurses give me IV fluids Thursday and Friday.
My heartrate stayed high for longer this time around: Thursday morning I checked it at 120. It made up for lost time Friday morning, though: I checked it at 44 beats per minute. I had the buzzing in my ears when I got up at night, like last cycle, and a dizzy spell Friday morning, again like last cycle. Only this time, the dizziness lasted longer and was complete with colored spots completely obscuring my vision. This repeated Saturday morning, with it taking a few hours before I was confident in my ability to stand up and stay that way.
I have slept more this weekend, my first "break" weekend, than in any previous cycle. Not only was there no early am insomnia Saturday - but after napping Friday and sleeping in Saturday, I went to bed at seven Saturday night and took a nap today, too.
I had hot flashes really badly while getting my seventh cycle of chemo. Multiple times every day and every night. I had night sweats when I was first diagnosed and for several cycles into treatment. They were intermittent; not having them often, plus the temperature changes as spring has come, I wasn't sure if the hot flashes were the same thing. But with the sweats, I didn't feel extremely hot. And with the hot flashes, I'm not extremely sweaty. So I think they're different. I have wondered if the hot flashes are related to my menstrual cycles: I have not ovulated since the end of January. I don't know if my fertility will come back post-chemo or not. The partner and I didn't have any plans for children, but the idea of that option being taken away is sad.
For now, though, I'm celebrating the disappearance of constant unbrushed or chalky tastes in my mouth: my husband and I went out to celebrate our sixth wedding anniversary. Yay us!
Friday, May 15, 2009
7 Quick Takes (lymphoma edition)
 I am addicted to message boards, ever since I discovered the (now-defunct) Estronet community nine years ago. I've moved from board to board as the internet communities and my life has changed. My most recent shift came in December, when I was diagnosed with cancer: I moved from the Long Hair Boards to the no hair boards.
I am addicted to message boards, ever since I discovered the (now-defunct) Estronet community nine years ago. I've moved from board to board as the internet communities and my life has changed. My most recent shift came in December, when I was diagnosed with cancer: I moved from the Long Hair Boards to the no hair boards. In the winter, when I most missed having hair: when lying down on my back, and the back of my head touched a cold pillow. I can't see my head (out of sight, out of mind) and putting on a bandana or scarf has comfortably replaced fixing my hair as part of my daily routine. But that cold touch on the back of my head got me every time.
In the winter, when I most missed having hair: when lying down on my back, and the back of my head touched a cold pillow. I can't see my head (out of sight, out of mind) and putting on a bandana or scarf has comfortably replaced fixing my hair as part of my daily routine. But that cold touch on the back of my head got me every time.While my head hair fell out after my first chemotherapy cycle, other facial hair waited until the weather got warmer. Now that cold pillows are no longer a concern:
- Not having eyelashes makes putting contacts in more of a challenge.
- I now need tissue for even the tiniest of sniffles. Not having nosehair, even the smallest amount of mucus runs straight out.
My husband baked cookies last week - and almost burned them. They're pretty hard, and he has apologized to me several times. The apologies were unwarranted, though: they turned out to be the perfect cookies for this week. Chemotherapy damages taste buds, and I have an aversion to sweetness. The cookies have had just enough of their sugar denatured that I can actually enjoy them. Anything that tastes good is precious to me right now, so hooray for almost-burnt cookies!
Humor has been a big help in keeping my spirits up. Following my first cycle of treatment, I was just feeling blah. My treatment regimen includes a high dose of steroids, and after I stop them I have a several day energy crash. "I don't feel good," I complain to my husband. He looks really concerned. "I've been thinking," he says. "Maybe you don't feel good because you have cancer." I laughed, as much as I could manage with my low energy. After that I felt a little better.
I am tired of eating Metamucil's fiber wafers. My daily dose of sugary, cinnamony, crunchy cookie goodness keeps my abdomen from causing me trouble, but it just gets hard to take eating the same thing day after day after day for four months now. I still have another few months of chemotherapy-damaged intestines, though, so Metamucil will get some more of my business.
I hope everyone is having a good Friday!
Monday, May 11, 2009
Beautiful
I was thrilled when my oncologist called my latest CT report 'beautiful'. He was very happy with how much the mass in my chest has shrunk.
Tumor size March 26, 2009 (measured by Dr. D):
* 6.7cm x 3cm on the axial projection (side to side & front to back)
* 5.3cm coronal measurement (top to bottom)
Tumor size March 26, 2009 (measured by Dr. C):
* 6.6cm x 3.9cm on the axial projection
* No coronal measurement given
Tumor size May 7, 2009 (measured by Dr. C):
* 4.3cm x 1.4cm on the axial projection
* No coronal measurement given
Since the tumor is still responding to the chemotherapy, we're going to do two more cycles, bringing my up to eight cycles total. Eight cycles will be it: one of the chemo drugs has a lifetime maximum dosage which I am close to (going over the lifetime maximum carries a high risk of heart failure). After I finish the chemotherapy, my oncologist said he'd like to send me to a lymphoma specialist to discuss whether or not I should do radiation.
From my own research, there is good evidence that radiation after chemotherapy reduces the risk of a relapse. However, it also carries risks of secondary cancers (because of my age, sex, and the tumor location, breast cancer would be of particular concern) and because my tumor is so close to my heart, heart damage from the radiation would also be a concern. It's not clear which option (rads vs. no rads) has a better risk/benefit analysis.
I know my doctors will make the best decision based on the evidence we have available. Regardless of which treatment plan we decide on, my chance of a cure will be good. And that's about all I can ask for.
Sunday, May 10, 2009
A bridge story
I've had a recent visit from each of my parents. With both of them, we ended up driving past one of the bridges in my town that is closed. I explained that we couldn't cross that bridge because a a train ran into it.
Most people have heard of trucks running into bridges. Which, to some degree, is understandable: drivers not familiar with the routes, or driving a semi taller than they are used to. Stuff happens. But a train? This railroad has gone under that bridge for over 100 years. That a train would have cars tall enough to hit it is kind of mind-boggling. Not to mention annoying, as that was the bridge I most frequently used.
Still, it makes for a good story to tell to visiting relatives.
Sunday, May 3, 2009
Double hung
As part of our remodeling, we've had most of the windows in our house replaced. Our reasons for replacing them were typical and not very interesting: to reduce heat loss and to make cleaning the outside of the windows easier.
What I didn't expect to appreciate with the new windows was their being double-hung. Our old windows, while all completely operable (surprising considering their age), had their top sashes painted shut. With the new ones, the top sashes work.
Since our downstairs rooms are works in progress, we don't sit around in them at all. When we're in those rooms, we're standing. Opening the bottom sash blocks the eye-level view from a standing height. Opening the top sash (newly possibly with the new windows) makes the outside more visible from a standing height. I'm finding it very nice; it's like the icing on the cake of these beautiful days we've been having.
So, hurray for double-hung windows.
Saturday, April 25, 2009
Morning birdsong
This morning I had my usual day 5 of cycle early a.m. insomnia. Laying in bed, deciding whether to get up or not, I heard a whippoorwill. I have never seen or heard one before, but the song was quite distinctive. And according to a short but seemingly well-referenced Wikipedia article, they are nocturnal birds whose range includes my location.
Hearing that song just made my morning.
Human granulocyte colony-stimulating factor
After my five days of chemotherapy, I get Neupogen (also called G-CSF) to help my bone marrow recover its ability to make neutrophils (bacteria- and fungus-eating white blood cells). White and red blood cells (among others) grow in several steps from stem cells; the chemotherapy does not kill the stem cells or the adult blood cells, but rather the steps in between. Adult blood cells normally die and are then replaced by younger ones; with chemotherapy disrupting the pipeline, though, blood counts drop lower and lower until the stem cells have had enough time to start over from scratch. The day with the lowest counts is called a nadir.
I get the Neupogen (subcutaneous in my abdomen area) every day until after my neutrophil nadir. My ANC (absolute neutrophil count) is always lowest on day 12 of my cycle, which works out to nine shots of Neupogen (cycle days six through fourteen). I suspect I'm actually good to go after eight shots. But confirming that would involve having bloodwork done on a Sunday, which I have not been motivated to pursue.
Last week, I came across this article on the EPOCH-R regimen, which says, "The ANC nadir was invariably observed around day 10–12 of treatment." Now I feel kinda behind the curve: having my nadir on day 12, when others are able to get that over with by day 10.
Neupogen has been on my mind more often lately, as just last cycle I did some of the injections myself. My oncologist's office normally has the nurses give all the shots, so I trekked into the office every day I needed the injections (including two weekends of each cycle). My last two shots of cycle five, though, I asked to take home and give to myself, and I'll do the same for these two weekends of cycle six. It's kinda neat to have a bag labeled "biohazard" in my refrigerator (the shots have to be kept chilled).
The manufacturer's directions for injecting Neupogen warn of hitting a capillary. If this happens, they say to discard that syringe and try again. My oncology nurses don't do this, they haven't had any adverse events from it, and at $350 per syringe I can understand the failure to follow this recommendation. The manufacturer's directions also specify either a 45º or 90º angle for the injection. All but one of my oncology nurses gives it at a 90º angle; after some experience with the 45º method, I found that it was more painful. So my own technique is the same as that of most of my oncology nurses: alcohol swab, straight in 90º, give the injection without checking for blood return.
It's fun to get the hang of this stuff, but I will be so glad when it's all behind me. I hope that time comes soon.
EPOCH+R, round six
In my second and third cycles, my heart rate would stay around sixty during my five-day chemotherapy infusion, then climb up a little over one hundred for a week, then drop back down to the eighties before my next treatment.
In cycles four, five, and six, my heart rate has been much more variable during chemotherapy (sometimes as low as sixty, still, but other times as high as 120). And in the week after (at least in cycles four and five), I've occasionally found my resting heart rate at 150.
I complained about this to my oncologist, and also let him know that light workout tapes bring my heart rate into the 170-180 range. He said he'd like to see my heart rate stay under 120. If my resting heart rate is elevated, he recommended nothing more strenuous than walking. He also sent me for an ECG and echocardiogram (ultrasound of my heart), both of which were fine.
I'm not thrilled with the high heart rate and my onc's disapproval, but the ECG and echo results are reassuring. Considering how much better I've felt these past few weeks (versus the previous weeks when I skipped exercising), I can't see myself giving up my workout tapes.
My onc did say that dehydration can contribute to an elevated heart rate. I've been having swallowing aversion and resulting low fluid intakes during my first break week; my first break week is also when my heart rate is the highest. Interesting. I don't know if my subconscious decided to run with that suggestion or what, but my fluid intake during treatment this week was 11-12 8-oz glasses a day. It hasn't been that high since my very first cycle; I was surprised at how consistently thirsty I was every day. It seems likely I'll have the swallowing aversion again this coming week; if so, I'm going to ask for IV fluids from my oncology nurses. That would be a simple enough thing to take some strain off my heart.
The increased fluid intake resulted in more nighttime restroom trips; the past few days these have been accompanied by buzzing/ringing in my ears (not the typical single tone of tinnitis, but more like a rainstorm). Friday morning when I first got up for the day, the ear sound was particularly strong, and I actually felt faint, which has not happened at any other time in my treatment.
Back to planning for the near future, I now have a numbing mouth wash to use for tongue pain. It seems likely it will again been severe enough to interfere with talking and eating painful. Apparently this kind of tongue pain is called stomatitis, although most texts discussing stomatitis talk about mouth sores (which I have not had). An article on EPOCH-R says stomatitis was "uncommon", but it happened enough to make their toxicity table, at 12% of cycles. The text of the article says stomatitis typically occurred in later cycles, which has been my experience. The Oncology Nursing Society says stomatitis may correspond with the white cell count nadir (lowest number of white cells), which has also been my experience.
Other things to look forward to this week: general weakness and bone pain. I think the weakness is what is called a "steroid crash". Lymphoma patients getting a more common regimen called R-CHOP get chemotherapy for one or two days, except for the steroids which are given for five days. They typically have lots and lots of energy and sleep very little on the steroid-only days; when they stop the steroids, they crash. I get chemotherapy for all five of my steroid days, so I don't really get the steroid "high". But I think stopping the prednisone still makes my body go, "What? I have to make my own steroids now?" and my increasing weakness these next few days is a "crash".
The bone pain last cycle was not nearly as severe as cycles one and two (before my chemo doses were escalated). But it woke me up for four nights in a row to take more pain meds; in cycles three and four taking 1300mg of acetaminophen before bed lasted me all night long.
Whew. I think I'm written out on chemotherapy for a couple of weeks (this blog has been a helpful therapeutic tool). On to happier things!
Monday, April 20, 2009
We have a roof!
Well, OK, the roof on our south living room was up two weeks ago. But I just now got around to posting the pictures, so here they are:


In the lower picture, the sunny spot to the left is our new back door (we won't have to go through the kitchen to get to the back yard!). The middle area will house a woodburning stove, and the room to the right is a competitor for world's smallest 3/4 bath.
Our porch rebuild is also still in the framing stage:

And we have a bay window in the kitchen:

I had the azalea (in back of the photo) for not quite three months before I killed it. Let me recommend the cyclamen (the one with flowers) to fellow brown-thumbs, though: it has managed to not only survive my ministrations the past five years, but bloom through them.
Back to the topic of roofs: our contractor has now fixed the damage from a tree falling on our house last summer (broken eaves, mangled gutters, damaged shingles). Since it rained all day yesterday, I was very appreciative of having gutters that worked.
I'm quite happy with how far our contractor has come in the six weeks they've been working. Maybe six more weeks and they'll be done? I guess I'll just have to wait and see!
Saturday, April 11, 2009
Meow?
I think people tend to compare growths in our bodies to spherical objects. A coworker who had a painful fatty deposit in his upper arm described it as golfball-sized. Another coworker whose wife passed from ovarian cancer described the tumor at the time of diagnosis as grapefruit-sized.
My tumor was never really even sort of spherical. I was describing it as pear-shaped after my first meeting with my oncologist, due to it being thinner in front of my heart and thicker to the right of my heart. My father has described it as potato-shaped when giving updates to his relatives.
After my last CT scan, I was describing the current dimensions to the partner. "I had a CAT scan," I said. "Meow meow cat scan?" he asks. "Was it bigger than a mouse?"
That conversation lasted all the way through dinner. We decided that while it was very much shaped like one, it was bigger than a mouse. Still, it is smaller than a hamster.
The kind of cancer I have leaves scar tissue behind; I will always have a residual mass. Now I'm going to go through life with the image of a small rodent having made a home in my chest. Ha. Thanks, husband.
Tuesday, April 7, 2009
Ballpoint idealism
In high school I was a cashier at a Dip 'n Dots stand. I never had to bring anything to work except myself; my supplies were at work. Including pens. During my first two summers of college, I got internships. Pens were always around.
The summer after my junior year, my pen ran out of ink, and there weren't any other pens. I started asking the supervisors for a pen, and ended up going around the entire office of four or five engineers. One of them did scrounge up a writing utensil for me, but it really was scrounged - out of the drawer of an abandoned desk or something. Not out of a supply cabinet as I had expected. They all seemed amused that I was asking for a pen, too, and I realized that they brought their own pens to work.
I felt really strongly that my workplace should provide me with writing utensils, and it was a mild shock to realize that not everyone felt that way.
Since graduation, I have continued to use pens provided by my employers. I never had a repeat of that episode at my internship; pens have just been supplied.
This morning, I talked with the accounting assistant about the pens they have now: they skip. (I suspect due to the oil that gets on many of the documents we use.) For years, my company has offered gel pens that do not skip, but we're out. The assistant seemed distraught that the other pens weren't working for me: "But the gel pens are so expensive!"
I knew we were having financial difficulties; I hadn't thought about them as extending to office supplies. I don't want to feel like my need for a pen was the tipping point in our company's decline; her distress was almost enough to make me consider buying my own pens, as do a number of my coworkers.
I don't think I'm ready to give up that ideal. A woman's got to hold on to something during hard times, and apparently for me, that something is a ballpoint pen.
EPOCH+R, round five
During my second break week of round four, I never felt good as I have in past cycles. This run-down feeling continued into my infusion week for round five, and Monday, Tuesday, and Thursday I just dragged through. Why I felt good Wednesday and Friday I'm not sure.
Our living area was rearranged a few weeks ago due to our remodeling, and my exercise space was one of the victims. During my first three rounds, I did two or three easy workout tapes during each break week. Not exercising during my break in round four is a top suspect for why I haven't felt so hot the past two weeks. I got my husband to rearrange again so that I could get back on the exercise bandwagon. Hopefully this will make the next round easier on me.
My fluid intake has been low again this cycle. I complained of it to the nurses last week, and they started giving me a bag of saline while I waited for them to mix up a refill for my pump. My normal fluid intake is water and a variety of tea flavors (mostly herbal). On these days when my thirst isn't working right, I've found that flavored water, or just adding lemon juice to water, or having coffee instead of tea makes it go down a little easier. Still, it's a struggle to keep my intake at 3-4 8-oz glasses a day. During round four my thirst started working normally on Friday of my first break week. Having to think about fluids so much is tiresome, so I'm looking forward to drinking becoming an automatic habit again.
Keeping on top of nausea medications is important. Like round four, the IV medication they gave me in the afternoon plus a pill in the morning (promethazine) kept my stomach happy during round five. I forgot the morning pill one day though, and besides being uncomfortable at work all day, the IV meds didn't completely take, and I needed a pill that evening.
The Neupogen is making me a little more achy this cycle than last: it's mild, but I needed to take Tylenol to get to sleep last night. The painful swelling from the steroid withdrawal has not been as bad this time; I'm not sure why, but am grateful. The tips of my fingers feel sorta numb off and on, but no tingling and no pain, and the muscle cramps in my legs, feet, and forearms that I had the first three cycles seem to have resolved: I attribute this to my lowered dosage of vincrinstine in rounds four and five.
Currently, my esophagus tingles, my tongue hurts (not to chew or swallow, just a mild ache), and it hurts to take deep breaths. Of these, the esophagus tingling bothers me the most, and makes eating uncomfortable. I've talked to several of the oncology nurses about this (today, and also when the same thing happened last cycle), and they say no one has ever complained to them about esophagus tingling before. Theories include neuropathy (like the tingling in my fingers) and something to do with the vagus nerve (which has some relationship to swallowing... and also to heart rate, which my heart rate is over 100 most of this week). They say as long as it goes away (which it did last cycle) it's not anything to worry about. So now, just to figure out what to have for dinner.
Saturday, April 4, 2009
Putting the "DA" in chemo
As has happened as I complete most of my treatment weeks, I woke up around 3am this morning and could not go back to sleep. Going straight from sleeping 10-11 hours a day to insomnia is always somewhat jarring; fortunately, the insomnia has never persisted beyond this one day.
In the meantime, I've been trying to make the best of it by doing research on the internet. I came across an interesting comment on the regimen I'm getting, which is a "dose-escalated" regimen (DA-EPOCH+R). If my blood counts (white cells, red cells, and platelets) tolerate a dose well, my next cycle I get more of the E,C, and H drugs.
According to this study, clearance of these chemotherapy drugs gets faster with successive cycles, especially in younger patients. Apparently our bodies can learn how to get certain poisons out of our system. Pretty neat. It does mean, though, that when we want poisons in our system (e.g. for cancer treatment) that it makes sense to increase the dosage over time.
So, my insomniac brain just thought I would share.
Monday, March 30, 2009
Making progress
I met with my oncologist today. My CT scan last Thursday showed improvements:
* The mass on my left adrenal gland is gone
* The pericardial effusion (fluid around my heart) is gone
* The tumor has shrunk some more
The shrinkage was not as much as I had hoped for. The measurements also seem to be dependent on which radiologist looks at them.
Tumor size February 11, 2009 (measured by Dr. O):
* 7.2cm x 3.8cm on the axial projection (side to side & front to back)
* 5 cm coronal measurement (top to bottom)
Tumor size February 11, 2009 (measured by Dr. D):
* 8cm x 4cm on the axial projection
* No coronal measurement given
Tumor size March 26, 2009 (measured by Dr. D):
* 6.7cm x 3cm on the axial projection
* 5.3cm coronal measurement
So just 1cm shrinkage in each axial direction, and no change in the coronal plane. Not nearly as encouraging as my first progress scan.
The type of lymphoma I have often leaves a mass of scar tissue even when all the cancer cells are killed - but 7cm would be a highly unusual amount of scar tissue. I was hoping for enough shrinkage we could possibly say the cancer cells were dead, and I'd only need two more chemo cycles (six total).
But since the tumor is still good-sized, I'll need more treatment after my sixth cycle. We'll do another CT scan: if the tumor has shrunk more, we'll do two more cycles (eight total) and evaluate from there. If it's the same size, we'll talk about other treatment options, probably radiation.
As disappointing as it is to be looking at months more of treatment, I feel so lucky I have a variety of effective treatment options available to me. Just thirty or forty years ago, I would have been dead within a year of diagnosis. So, hooray for effective chemotherapy, and on to cycle five.
Friday, March 27, 2009
Dancing floor

For nearly three weeks, the door from our dining room has opened onto a three foot drop. Yesterday, the floor of what will be our new living room was installed. Excited that there was something solid outside the dining room door, I opened the door and walked out shortly after getting home. "Congratulations on your new dancing floor," says our carpenter.
Sunday, March 22, 2009
EPOCH+R break four: side effect round up
While my bone marrow tolerated the increased dose in cycle three very well, this doesn't appear true for the further dose increases in cycle four (dose increases were for the E,C, and H drugs). Hemoglobin is a component of red blood cells: levels of less than 12 are considered anemic, less than 8 require a blood transfusion. I've been between 9.5 and 10.5 since my first chemo cycle; on Friday my hemoglobin was 8.4. Neutrophils are a kind of white blood cell needed to fight bacterial infections; absolute neutrophil counts (ANC) below 1000 are considered dangerous. My first cycle, I dropped below 1000, but not in cycles two and three. Friday, though, my ANC was 144. I don't think my oncologist will be increasing my dosage for cycle five.
Despite a reduction in dose of vincristine, the O drug, the tingling/numbness in my fingertips came back the Sunday after my fourth round. It's still here a week later. But, it has not spread any further up my fingers, and they don't hurt nearly as easily.
Also on Sunday, I got a tingling sensation at the very top of my breastbone when I ate. With each swallow, the tingling sensation would spread out to a larger area. Not that the tingling was particularly unpleasant, but for some reason I developed an aversion to swallowing, especially liquids. And the underside of my tongue hurt - the pockets where you stick a thermometer. Chewing was fine, but extending my tongue to clean food from the outside of my teeth was extremely painful (so I've been using my fingers to get food out from in between teeth).
On Wednesday, that area at the top of my breastbone hurt all day, especially when taking deep breaths. Wednesday night, by the time I finished dinner, the tingling had spread to my ears. My aversion to swallowing was strong enough I only managed three or four 8-oz glasses for my fluid intake that day. All these symptoms have gradually improved; by Friday only the tongue pain remained. Today (Sunday) my tongue hurts just a little - I can even use it to get food off my teeth again.
I'm guessing all of this is caused by the same kind of nerve damage that is causing the fingertip issues. When I told a nurse about my breastbone pain, she had one of the doctors come talk to me - his best guess was also neuropathy. I think being so bothered by my issues with swallowing has made me not be bothered by the weird sensations in my fingertips. I'm glad everything seems to be resolving fairly quickly. I hope next cycle isn't any worse.
Biopsy payment
When my tumor was biopsied in December, my insurance paid for the procedure at my local hospital, but not for the interpretation of slides done at the University of Iowa (which for some reason came as two separate bills). I called my insurance company, and was told the University of Iowa was out of network. That was discouraging.
I asked my oncologist's office about this, and they said, no, that wasn't right, they would resubmit the bills. A few days later, I got a slip from my insurance company that they were going to pay one of the bills. That was a big step in the right direction.
A few weeks went by with no word on the other bill, so Friday I called my insurance company. The agent was very confident that U of I was out of network, and that bill was not going to be paid. I pointed out the other bill (part of the same biopsy interpretation) that they had paid. No, she said, U of I was out of network, and they hadn't paid that. (!)
We went back and forth a few times, she insisting it hadn't been paid, me insisting it had. On March 3rd it was paid, I told her, find an action on that claim on March 3rd. February 18th, March 2nd... then she found March 3rd. There was silence for a minute. I was really afraid she was going to find something to un-pay it.
Then a light bulb must have gone off. "Did you go to the University of Iowa?" No, my biopsy was done at my local hospital. Only the slides were sent to U of I. Well, that was entirely different. Of course they would pay. She apologized for the trouble they had caused me.
Good news, but how bizarre. I would have thought the thousands of dollars in hospital bills would have clued them off that I was in my local hospital that day. Or that the procedures being billed from U of I would have obviously been done on slides, not an actual person. Considering all the money that passes through their system, health insurance does not seem as with-it as one would hope.

